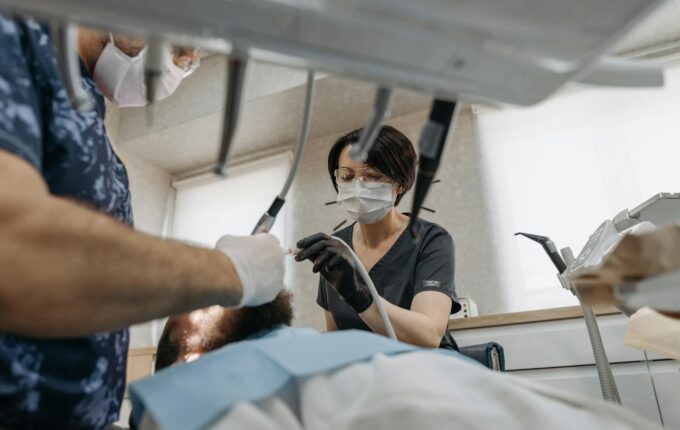
Tips for Recovery from Gum Grafting

Proper postoperative care is essential for a smooth recovery. Learn how to manage discomfort, understand the healing stages, and ensure the long-term success of your graft.
Board Certified Periodontists 5-Star Rated Insurance Friendly
212-355-2290 Book Consultation
Jump to: Recovery Tips | Healing Timeline | Types of Grafts | Prevention
Key Takeaways:
- Proper postoperative care is essential for a smooth recovery from gum grafting.
- Manage discomfort and get adequate rest to improve gingival graft healing.
- Avoid strenuous activities and get enough rest to support tissue integration and long-term success of the graft.
- Gum graft surgery recovery tips promote stability and healthy tissue during the healing.
One day, we look in the mirror, and our smile seems a little off. A tooth appears longer, and its base appears browner. If we drink something cold, it sends shock waves to our brain. Gum graft surgery will help improve these symptoms but having surgery means there will be recovery. Understanding protocol for recovery from gum grafting will help you maintain the results achieved with treatment.
Many patients are unaware of the stages of gingival graft healing and how the tissue gradually strengthens over the first few weeks. However, they can learn that there are several types of grafts depending on the severity of the recession.
Here, we’ll explore the different types and healing stages to help you prepare for a successful recovery.
Practical Gum Graft Recovery Tips
Proper care immediately following your procedure is crucial for the stability of the new tissue. Following basic gum graft surgery recovery tips helps patients feel more comfortable during this phase.
Medication & Pain Management
To prevent post-op infections, we usually prescribe a seven-day course of antibiotics. Manage mild discomfort by alternating Tylenol Extra Strength and ibuprofen (Advil). Use analgesics as directed so you can return to work the same day or the day after.
Swelling & Bleeding
Apply ice to the surgical area to prevent swelling. Alternate ten minutes on and off for one to two days. To stop bleeding, use sterile gauze with light pressure. Moistened tea bags containing tannic acid can also help. Note that light oozing is normal for the first two days.
Diet & Hydration
Drink lots of liquids to hydrate the body during healing stages. Stick to soft foods; avoid stiff, scratchy, or acidic foods (like citric juices) that disturb the surgical site. Avoid hot and cold foods immediately after surgery.
Oral Hygiene
Good hygiene is vital, but be gentle. You can brush teeth in non-surgical sites the day after. NO flossing for two weeks. Gently lavage the mouth 2x daily with Peridex Rinse. Do not disturb the surgical sites with trauma.
Rest & Position
Rest is a great healer and plays a significant role in successful recovery. Prioritize sleeping on your back or side with your head elevated. No strenuous exercise for two weeks, though walking and desk work are encouraged.
Surgical Protection
A palatal stent is used occasionally with free types of gingival grafts to protect the donor site. Always follow specific instructions regarding any protective devices.
Stages of Gingival Graft Healing
Many patients are unaware of the stages of gingival graft healing and how the tissue gradually strengthens over the first few weeks. Here is what you can expect.
Recovery Journey
Days 1-3: Stabilization
Patients usually notice most recovery symptoms in the first two or three days. Mild swelling and normal tenderness appear as the new tissue stabilizes. Cold compresses and head elevation make this part of the process more comfortable.
Day 4-7: Settling
The graft can look lighter and slightly pale by the end of the first week. This is normal. The tissue gradually blends in as blood flow increases. Most people notice less sensitivity and fewer temperature-related reactions around this time.
Week 2: Strengthening
By the second week, the graft begins to strengthen. Sutures may be removed, and brushing can resume in non-surgical areas. Avoid flossing near the graft. Healthy surrounding tissue supports long-term recovery and integration.
Types of Grafts & Procedures
One day, we look in the mirror, and our smile seems a little off. A tooth appears longer, and its base appears browner. This condition, known as receding gums, often leads patients to seek recovery from gum grafting later.
Candidate Assessment
Our board-certified periodontist, Dr. Jin Wang, diagnoses your recession. He determines if you have sufficient interproximal bone, which supplies the necessary blood flow to the graft. This evaluation ensures that the procedure and subsequent gingival graft healing stages progress smoothly.
The Surgical Procedure
A local anesthetic is administered to numb the surgical site(s). Nitrous oxide is also available if needed. Dr. Wang carefully harvests tissue and attaches it to the affected area. You’ll learn what to expect during the recovery so you know how the area should look as it heals.
Common Grafting Techniques
Connective Tissue Graft
This is our most common graft, used when recession is moderate. It increases the length and thickness of gingival tissue. The donor tissue comes from under the patient’s palate skin, meaning there is no open wound on the roof of the mouth. This method usually moves through healing stages with fewer color changes.
Free Gingival Graft
Used when recession is severe or there is no keratinized tissue. We take the outer covering and deeper connective tissue from the upper palate. Once this graft is in place, it prevents further bone loss. The donor site on the palate heals in about 1 to 2 weeks.
Pedicle Graft
A good choice when recession involves a single tooth. Dr. Wang rotates tissue from a neighboring tooth and sutures it into the defect. Because the tissue remains partially attached to its original blood supply, this method tends to yield a steady, predictable recovery.
Alloderm Graft
The least invasive type, as it comes from a donor other than the patient. The palate is not used. The new graft is sutured into place at the recession site, causing minimal post-op discomfort.
Causes & Prevention of Receding Gums
Receding gums affect up to 10% of the population. Delaying treatment can lead to decay, bone loss, and eventual tooth loss.
Causes of Recession
- Bruxism: Grinding wears down teeth and imposes horizontal force that shrinks gum and bone.
- Poor Hygiene & Diet: Plaque formation and sugar/acidic foods damage supporting structures.
- Aggressive Brushing: Horizontal forces and abrasive “whitening” toothpaste abrade gums.
- Genetics & Age: Recession incidence increases as we get older due to cumulative trauma.
- Misalignment: Severe misalignment can benefit from grafting once tissue has receded.
Prevention Strategy
- Routine Exams: Checkups and cleanings twice a year with X-rays.
- Proper Brushing: Use a soft-bristle brush (like Sonicare) for 2 minutes twice daily.
- Night Guards: A noninvasive way to eliminate harmful grinding effects.
- Orthodontics: Invisalign braces align teeth to eliminate horizontal forces.
- Healthy Diet: Prioritize low-sugar foods and Vitamins A and C.
Book an Appointment with 209 NYC Dental
If your gums are receding, your smile looks awkward, and you are experiencing sensitivity to hot and cold, you may be a candidate for gingival graft surgery. Don’t delay, call 209 NYC Dental and make a consultation with our general dentists.
Many patients find that early evaluation leads to a smoother, more predictable recovery after gum grafting.
Call 212-355-2290 Schedule Consultation
209 NYC Dental
209 East 56th Street, 1st Floor
New York, NY 10022
 Our History
Our History
 Our Providers
Our Providers
 About Us
About Us
 Blog
Blog
 Contact us
Contact us
 Diagnostic & Preventive
Diagnostic & Preventive
 Dental Implants
Dental Implants
 Clear Braces - Invisalign
Clear Braces - Invisalign
 Cosmetic Dentistry
Cosmetic Dentistry
 Periodontics
Periodontics
 Patient Forms
Patient Forms
 Payment Information
Payment Information
 Insurance Options
Insurance Options
 CareCredit Dental
CareCredit Dental
 Appointment Policy
Appointment Policy
 Free Consultation
Free Consultation
 Complimentary Teeth Whitening
Complimentary Teeth Whitening
 Teeth Whitening
Teeth Whitening