Periodontal Disease (Gum Disease): A Silent Threat to Your Health

Did you know that, according to the American Dental Association, nearly 50% of adults in the U.S. are affected by periodontal disease? This silent disease is often overlooked and can have serious consequences to your overall health.
In this article, we will cover periodontal disease treatments, causes, symptoms, risk factors, and why consulting an expert is recommended when symptoms appear. 209 NYC Dental offers a range of periodontal therapies performed by our board-certified gum disease specialists.
What is Periodontal Disease?
Periodontal disease (also known as gum disease) is a serious bacterial infection that triggers inflammation in the gums and damages the bone surrounding the teeth. It typically begins as gingivitis and, if left untreated, progresses to periodontitis, which can lead to tooth loss.
What Causes Periodontal Disease?
Many patients wonder what exactly triggers these infections. While plaque is the most common culprit, other causes of gum disease include genetics, chronic illnesses, and certain medications that reduce saliva flow.
Saliva helps wash away bacteria, so when production slows, microbes multiply faster. Environmental stressors such as poor sleep, smoking, and dehydration can also make gums more vulnerable. Understanding these lesser-known causes of gum disease helps patients take proactive steps before inflammation ever begins.
Progression of Gum Disease
Gum Disease starts when plaque, a sticky bacterial film, forms on your teeth, and when not removed during brushing, hardens into tartar or calculus. As tartar builds up, it irritates the gums, causing puffy, inflamed gums.
As the infection gets worse, the gums recede, forming pockets that trap bacteria. This is called “pocket formation”. A hygienist measures pockets with a periodontal probe, a “dental ruler” with 1mm gradations. In a healthy patient, we find a space of 1 mm to 3 mm between the tip of the gum and where the gum attaches to the bone. As periodontal disease advances, we see pockets measuring 5mm-7mm, which severely compromise the health, stability, and ultimately the retention of the tooth.
As the pockets get bigger, they get infected. That can cause loose or sensitive teeth and more gum tissue and bone destruction, which can also change the way your teeth fit together when you bite.
If not managed with gum disease treatments, periodontal disease can progress and lead to tooth loss.
To prevent or manage periodontal disease, it is essential to maintain good oral hygiene. Regular dental cleanings with a hygienist are necessary to prevent tartar buildup and maintain healthy teeth and gums.
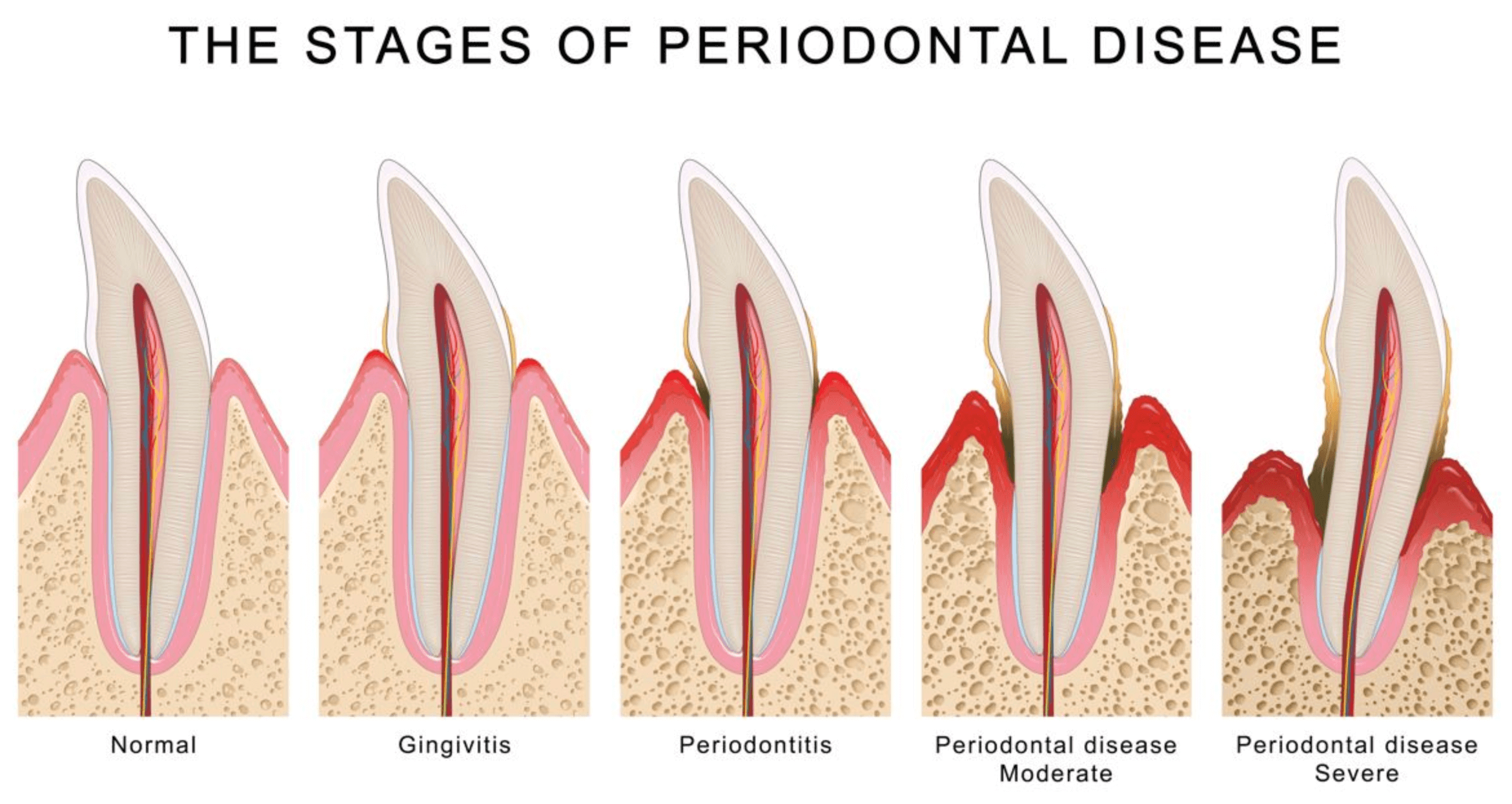
Stages of Gum Disease
Gum disease is a silent yet potent threat to oral health. It progresses through distinct stages of gum disease. Knowing these stages is key to early detection and intervention.
Gingivitis
The first stage of gum disease is called gingivitis. It causes inflamed, red, tender, and swollen gums. This inflammation is a response to bacterial plaque, a sticky film that forms on your teeth. Gingivitis is the mildest form of periodontal gum disease, but if left untreated, it can progress to a more severe stage of gum disease.
Periodontitis
Periodontitis is a more advanced form of periodontal disease that involves the destruction of the tissues supporting the teeth. As the infection deepens, it begins to erode the bone that holds teeth in place. This can lead to a variety of dental issues, including:
- Pocket formation and bleeding gums: As the gums recede, pockets form between the teeth and gums. These pockets harbor bacteria, making them difficult to clean. Bleeding gums often accompany this stage of gum disease, serving as a warning sign of periodontal disease.
- Bone loss: The destructive nature of periodontitis can lead to significant bone loss, weakening the teeth and increasing their susceptibility to loosening.
- Tooth loss: In severe cases, periodontitis can result in tooth loss.
Gum disease specialists can further categorize gum disease stages by assessing the severity of bone and tissue damage, from mild to advanced periodontitis. These diagnoses will guide appropriate professional treatments for gum disease.
It’s important to note that the progression of periodontitis can vary from person to person. Factors such as dental hygiene practices, systemic health conditions, and genetic predisposition can influence the rate of disease progression. Early detection and prompt treatment are crucial for preventing the disease from worsening and preserving dental health.
If you notice any warning signs and symptoms of gum disease, don’t hesitate to schedule a consultation with a periodontist at 209 NYC Dental. Early diagnosis and professional treatment can stave off the progression of gum disease and help maintain your oral health.
Signs and Symptoms of Gum Disease
Early signs of gum disease, such as gingivitis, can be subtle and often go unnoticed. However, as the disease progresses, the signs become more noticeable. Keep an eye out for these red flags:
- Bleeding gums are an early sign of periodontal disease. Even gentle brushing can cause bleeding.
- Swollen, red, or tender gums
- Persistent bad breath: Gum disease can cause bad breath that persists even after brushing and flossing.
- Receding gums: The gum tissue can pull away from your teeth, exposing the roots.
- Pain or discomfort when chewing: Periodontal disease can cause sensitivity and pain when eating due to exposed roots.
- Changes in bite: As teeth loosen and move, your bite can shift.
- Loose teeth: As bone loss progresses, teeth can become loose, and patients may require extraction and bone grafts to restore lost bone.
It’s essential to acknowledge that the signs and symptoms of gum disease don’t always follow a consistent timeline. Some people experience bleeding first, while others notice subtle swelling or sensitivity to cold. Another overlooked indicator is that teeth may appear slightly longer than before. That’s a sign of an early gum recession.
Using clinical photos or educational images of gum disease can help patients identify problem areas early. In advanced stages of gum disease, the gum color can shift from pink to red or even purplish, indicating restricted blood flow.
If you experience any of these warning signs, it’s important to see a dentist or periodontist for a full gum health assessment. Even minor gum irritation or persistent odor can point to damage beneath the surface. Periodontal checkups and diagnostic images taken during cleanings help reveal issues early, when treatment is most effective.
The Importance of Gum Health
Gum health is crucial to overall oral health and the prevention of periodontal disease. Healthy gums are firm, pink, and fit snugly around the teeth. They support the teeth and protect the underlying bone and tissue. Healthy gums help:
- Stop plaque and bacteria from building up on the teeth: Healthy gums act as a barrier against harmful bacteria. Additionally, if left unremoved, plaque can lead to tooth decay.
- Prevent gum recession: Receding gums are not only aesthetically unappealing, but they are also a precursor to dental pathologies such as root caries and periodontal gum disease.
- Reduce the risk of periodontal disease and loose teeth.
- Support the teeth and keep them in place: They provide the support to keep teeth in their proper position.
- Enhance your smile: Healthy, pink gums lead to a beautiful smile.
Risk Factors for Gum Disease
Gum disease can affect anyone, but certain risk factors increase the likelihood of developing the condition. These include:
- Poor oral health: Neglecting regular brushing and flossing can lead to plaque buildup.
- Misaligned teeth: Crowded and crooked teeth, spaces between teeth, and other dental misalignments can create hard-to-reach areas in your mouth. These spaces often become breeding grounds for plaque and bacteria, increasing the risk of poor oral hygiene.
- Smoking: Tobacco use is a significant cause of gum disease.
- Diabetes: High blood sugar levels can contribute to the development of periodontal disease.
- Heart disease: A link exists between gum disease and cardiovascular conditions.
- Obesity: Excess weight can increase the risk of periodontal disease.
- Stress: Chronic stress can weaken the immune system, making it harder to fight infections.
- Hormonal changes: Pregnancy, menopause, and other hormonal changes can affect gum health.
- Genetics: A family history of gum disease can increase your risk of developing gum disease.
- Age: Gum disease signs and symptoms are more common among adults over 30.
- Certain medications, such as steroids and certain antidepressants, can affect gum health.
According to the Centers for Disease Control and Prevention (CDC), about 47% of adults in the U.S. have some form of periodontal disease, 9% of whom have severe stages of gum disease. It is more prevalent among smokers, people with diabetes, and obese individuals.
Gum Disease Treatment with Expert Periodontists
Modern gum disease treatments focus on reducing infection, protecting gum tissue, and preventing future damage. Depending on the severity of the condition, patients may receive deep cleanings, targeted bacterial control, or supportive home-care plans to maintain results between visits.
Dentists often emphasize the importance of consistent oral hygiene, regular checkups, and daily rinsing with an approved gum disease mouthwash to help manage bacteria and inflammation. These professional and at-home measures work together to slow disease progression and support long-term gum health.
Our experienced board-certified periodontists offer a range of dental treatments targeting gum disease:
Nonsurgical Treatment for Gum Disease
- Scaling and root planing (SRP): Also known as deep cleaning, SRP removes plaque and tartar from both above and below the gum line. By smoothing the tooth’s root surface, deep cleaning helps prevent tartar buildup and promotes gum healing.
- Laser therapy is a minimally invasive procedure that utilizes laser energy to kill bacteria and stimulate tissue healing.
- Antibiotic therapy: In some cases, antibiotics may be prescribed to target specific bacteria associated with periodontal disease.
Surgical Procedures
- Osseous surgery or flap surgery is a surgical procedure designed to reshape and repair bone tissue damaged by periodontal disease. By removing diseased tissue and reshaping the bone around the affected teeth, osseous surgery can help create a healthier environment for the gums to heal and recover.
- Bone graft: Bone grafting is a surgical procedure that involves replacing lost bone with a bone graft, using the patient’s own bone, donor bone, or synthetic bone. This procedure can help to regenerate bone and support tooth structure.
- Soft tissue grafts: Soft tissue grafts are a surgical procedure used to address gum recession. In this procedure, tissue is taken from another area of your mouth, often the palate, and grafted onto the affected area. Gum grafting in NYC also helps cover exposed roots, reduce sensitivity, and prevent further gum recession.
By combining these gum disease treatment options with a comprehensive approach to dental hygiene, 209 NYC Dental can help you achieve optimal dental health and a beautiful smile.
209 NYC Periodontists treat all gum related issues from gum infection emergency to chronic gum inflammation and bone loss.
Take charge of your health today!
Schedule Your Periodontal Consultation Today!
The Risks of Untreated Gum Disease
Gum disease is a significant public health concern that affects millions of people worldwide. According to the CDC, it is the leading cause of tooth loss among adults in the United States. Research has shown that periodontal disease has other risk factors and is linked to various systemic health conditions, including:
- Coronary artery disease: Gum disease can increase the risk of heart disease.
- Diabetes: A bidirectional relationship exists between gum disease and diabetes.
- Respiratory infections: Infections in the gums can contribute to respiratory problems.
- Rheumatoid arthritis: Chronic inflammation from gum disease can exacerbate arthritis.
- Stroke: Gum disease has been associated with an increased risk of stroke.
- Premature birth and low birth weight.
The American Dental Association estimates that gum disease costs the United States healthcare system over $50 billion annually. The National Institute of Dental and Craniofacial Research (NIDCR) conducts extensive research to understand better the causes, symptoms, and treatment options for gum disease.
How to Prevent Gum Disease and Reverse Gingivitis
While gum disease can be managed effectively in many cases, prevention is always the best approach. By incorporating proper daily oral hygiene habits into your routine, you can significantly reduce your risk of developing gum disease and even reverse gingivitis. Reversing gingivitis, the mildest form of gum disease, is possible with consistent and effective oral hygiene practices.
- Brush your teeth properly: Brush your teeth twice daily using a soft-bristled toothbrush and fluoride toothpaste, paying special attention to the gum line to fight plaque accumulation.
- Floss daily: Floss can access areas where toothbrushes cannot, such as tight spaces between teeth and near the gum line. Make it a habit to floss every night before bed.
- Use an antiseptic mouthwash for gum disease to reduce bacteria and maintain gum health. Look for a mouthwash with the American Dental Association (ADA) Seal of Acceptance.
- A healthy diet rich in fruits, vegetables, and whole grains can support your immune system. Limit sugary snacks and drinks, as sugar can contribute to plaque build-up.
- Drink plenty of water; it helps wash away food particles and bacteria, reducing the risk of gingivitis.
- Avoid tobacco products, as they’re some of the leading causes of gum disease.
- Visit your dentist regularly for professional dental cleanings to remove plaque and tartar buildup. Your dentist or dental hygienist can detect early signs and symptoms of gum disease.
If detected and treated early by following these steps, gingivitis can be successfully reversed and prevented from progressing to periodontitis.
Visit 209 NYC Dental and Experience the Difference
At 209 NYC Dental, we’re committed to providing exceptional periodontal care. Our board-certified periodontist, Dr. Jin Wang, brings decades of experience and expertise to every patient.
Whether you’re dealing with gum problems, missing teeth, or any other dental condition, our multi-specialty team is here to help.
- We offer a comprehensive range of dental services, including non-surgical gum disease treatments and surgical procedures such as scaling and root planing, guided tissue regeneration, dental implants, bone grafting, and soft tissue grafts.
- Convenient appointments: Our dental office offers same day appointments 7 days a week to accommodate your busy schedule.
- Dental Insurance: Our dentists accept most PPO dental insurance plans, making it easier for you to access the care you need.
- Reputation: We have thousands of reviews across the internet, all of which attest to the excellent dental care we provide in our NYC dental office.
We encourage you to schedule a consultation with a 209 NYC Dental gum disease specialist if you’re experiencing any symptoms of periodontal disease or have concerns about your oral health. Our experienced periodontists can provide a comprehensive evaluation, review your x-rays, offer information, diagnose any underlying issues, and recommend the most appropriate treatment plan for gum disease.
By understanding the stages of gum disease and taking proactive steps to maintain a healthy mouth, you can significantly reduce the risk of severe complications and enjoy a healthy smile for years to come.
Remember, a healthy smile starts with a healthy mouth. Take control of your health today and schedule your appointment.
Contact us today to schedule a consultation.
FAQ
Is periodontal disease contagious?
No, periodontal disease is not contagious. It is primarily caused by poor oral hygiene and the buildup of plaque and tartar on the teeth. While the bacteria that contribute to gum disease can be spread through saliva, the disease itself is not directly transmitted from person to person. Keeping your teeth and gums clean is crucial for preventing and managing periodontal disease.
Is gum disease curable?
No, it is not curable. However, it is manageable with gum disease treatment. Once structural support around teeth is lost, as in the case of periodontitis, it usually cannot be regained. With proper treatments and good oral hygiene, it is possible to prevent further damage and maintain stable gums and teeth. However, gingivitis can be reversed with professional dental cleanings and a diligent at-home oral hygiene routine.
 Our History
Our History
 Our Providers
Our Providers
 About Us
About Us
 Blog
Blog
 Contact us
Contact us
 Diagnostic & Preventive
Diagnostic & Preventive
 Dental Implants
Dental Implants
 Clear Braces - Invisalign
Clear Braces - Invisalign
 Cosmetic Dentistry
Cosmetic Dentistry
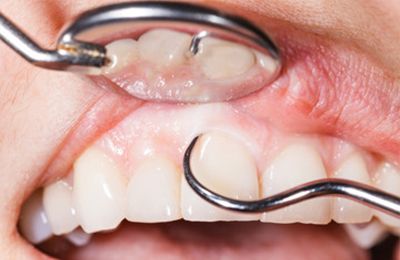 Periodontics
Periodontics
 Patient Forms
Patient Forms
 Payment Information
Payment Information
 Insurance Options
Insurance Options
 CareCredit Dental
CareCredit Dental
 Appointment Policy
Appointment Policy
 Free Consultation
Free Consultation
 Complimentary Teeth Whitening
Complimentary Teeth Whitening
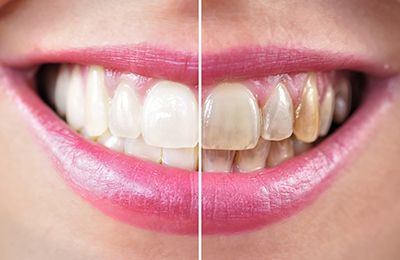 Teeth Whitening
Teeth Whitening